If you’re here, something may not feel quite right in your body. Maybe you leak a little when you laugh, or you feel tension that doesn’t fully release. Maybe you tried Kegels, hoping to fix it, but instead, things felt worse or more confusing.
So naturally, you’re wondering: Is my pelvic floor tight or weak?
I’m Coco Berlin, a certified pelvic floor expert, movement therapist, and former professional dancer. For over 20 years, I’ve worked with women around the world, helping them reconnect with this deeply important part of their body.
And here’s what I want you to know first: you’re not alone. This question is one of the most common I hear, and for a good reason: pelvic floor symptoms are very common. In the United States, a large study found that about 1 out of every 4 women has symptoms of a pelvic floor problem [1]. More recent data shows that over 60% of adult U.S. women experience some leakage [2].
But here’s where it gets confusing. It seems logical to assume there’s a simple answer: pain means tight, and leaking means weak. Fix one, and everything improves. But in reality, your pelvic floor doesn’t work like an on-off switch. It works more like a system: one that needs to lift, soften, and respond at the right time.
So here’s my short answer: most women are not just tight or weak. They are often both. A pelvic floor can stay tense all day and still feel unstable. It can feel strong, yet respond too slowly. It can leak and feel tight at the same time. That’s because the real issue is rarely strength alone, but a lack of functional integration and coordination.
In this article, I’ll guide you through:
The signs your pelvic floor struggles to relax
The signs it struggles to activate
How it can be both at the same time
Why self-tests can be misleading
And what actually helps
By the end, you’ll have a clearer sense of what may be happening in your body and what your next step could be.
How do you know if your pelvic floor is tight or weak?
For many women, their pelvic floor is not just tight or weak. Very often, it’s both.
If your pelvic floor is “tight” (also called overactive or high-tone), the muscles stay slightly braced, even when you’re resting. They don’t fully soften. You might feel guarded, numb, or “locked.” Sex or tampon use can hurt. Emptying your bladder may feel incomplete. You may also experience constipation or the feeling that you need to go but can’t fully “let go,” leading to straining, which can put even more pressure on the pelvic floor. And yes, you can feel tight and still leak.
If your pelvic floor is “weak” (underactive), the muscles don’t respond quickly or strongly enough. You might leak when you cough, laugh, or run. You may feel heaviness or pressure. When you try to activate your pelvic floor, it can feel unclear or hard to find.
Symptoms and self-tests can suggest patterns, but they cannot diagnose you. Only a structured pelvic floor exam can clearly tell the difference [3]. At the same time, women in my training learn how to understand what’s happening in their own body and trust it more.
Here’s what I often see in movement therapy: a muscle that is always gripping doesn’t get stronger. It misses the natural cycle of tightening and relaxing.
Over time, it gets tired, less coordinated, and can’t respond when needed. The tissue becomes stiffer, and timing gets worse.
The result is a pelvic floor that feels tight, weak, and unstable at the same time.
This is because pelvic floor health goes way beyond strength: it’s about coordination, timing, breath, and how safe your nervous system feels.
That’s why squeezing harder is never the answer. The body needs awareness first.
Your body isn’t broken, it has been adapting. And with the right holistic approach, it can find balance again.
If you’d like a gentle way to begin, I created a free 5-part mini course to help you reconnect with your pelvic floor step by step.
In just a few minutes a day, you’ll explore simple movements, breath, and awareness practices that help your body feel more relaxed, supported, and alive again.
You’ll also get access to a supportive community where you can share your experience and ask questions along the way.
Start the free BODY LOVE mini course here:
BODY Love
mini course
Start feeling amazing in your body today
Why This Question Is Harder Than It Sounds
To better understand why the tight-or-weak question can be misleading, it’s important to understand first how your pelvic floor works as a whole system.
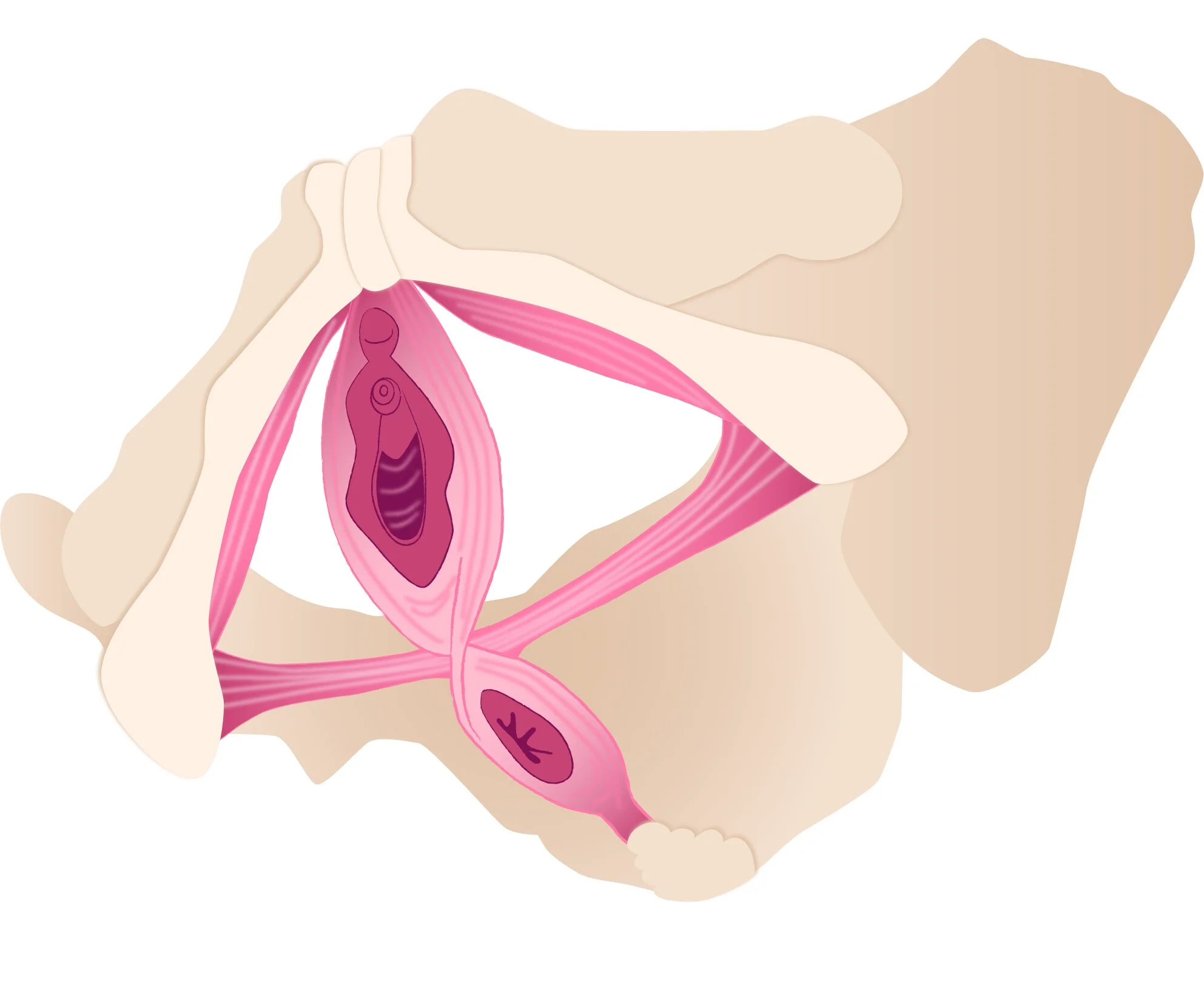
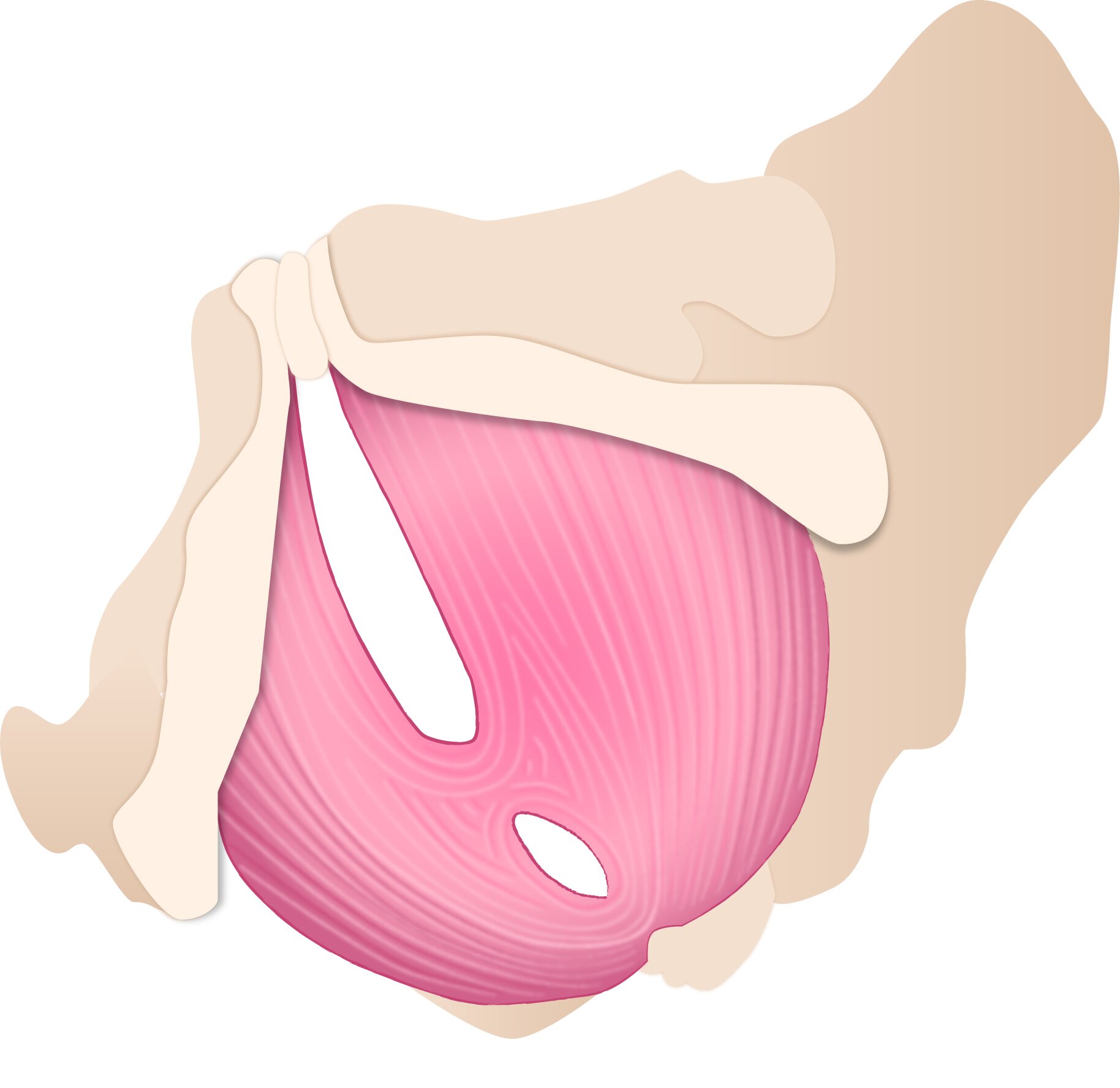
Your pelvic floor is a complex network, which can be structurally divided into three layers of muscles, all working together like a team. These layers are supported by connective tissue and filled with nerves and blood vessels. They hold your bladder, uterus, and bowels [4]. They gently lift and release as you breathe, and help you stay steady when you walk, bend, laugh, or cough. And like any good team, they work in a connected and coordinated way.
First layer
Second layer
Third layer
Pelvic floor muscle layers © Coco Berlin's book Pussy Yoga
Your pelvic floor works together with your belly, back, and diaphragm (your main breathing muscle). It responds to how you sit, stand, walk, and move throughout your day.
It also responds to how you feel. When you are stressed or tense, your pelvic floor may tighten without you realizing it.
This happens in other parts of the body too. Muscles like your jaw, diaphragm, or shoulders often hold tension during stress, and your pelvic floor is part of this pattern. Research shows that over time, this can change how your pelvic floor moves and responds, even if you’re not aware of it [5].
Over the years, I’ve noticed that many women carry this kind of quiet tension in their pelvis. It isn’t always obvious. It can go unnoticed and feel completely normal.
The muscles stay slightly braced, like they are holding something together. Over time, this reduces flexibility and timing. The pelvic floor may feel firm, yet still lack true support.
At the same time, many women struggle to feel this area clearly. I often hear:
“My pelvis feels like a black box.”
“I feel disconnected from my body.”
Imagine trying to play piano while wearing thick winter gloves. You can press harder, but you still won’t have fine control because you can’t truly feel the keys.
The same thing happens with your pelvic floor: you may try to squeeze harder during Kegels or “activate more”, but without sensory awareness of your entire pelvic floor network, it’s impossible to coordinate or train it properly.
When you can’t feel a part of your body, you can’t truly trust it. And over time, that can feel like being disconnected from yourself. This is why the tight-or-weak question can be misleading. The deeper issue is often integration: how well this system works with the rest of your body.
And that leads to the next important piece.
What Your Pelvic Floor Is Doing When You’re Not Thinking About It
Your pelvic floor is always working, even when you’re not aware of it.
For example:
Every time you inhale, your diaphragm moves down, and your pelvic floor gently lengthens and responds to the pressure.
When you exhale, it lifts back up.
This subtle, natural rhythm happens thousands of times a day without you having to control it.
Your pelvic floor also helps keep you steady. It supports your pelvis and spine when you stand in line, carry groceries, or turn to look behind you. When you cough, sneeze, laugh, or jump, it reacts in a split second to manage pressure inside your belly.
In a healthy pattern, the pelvic floor is responsive and adaptable. It can lift when support is needed and soften when it’s time to release. It stretches, rebounds, and moves in harmony with the rest of your body.
Now, imagine a different pattern. In an overactive state, the pelvic floor stays slightly gripped, even at rest. It’s like holding your fist half-clenched all day long. Over time, that steady tension reduces blood flow and dulls sensation. The area may feel tight, heavy, or harder to sense clearly.
In an underactive pattern, the issue looks different. The muscles have trouble responding when pressure increases. When you cough or land from a small jump, they may not lift quickly enough to provide support. The timing feels off, and stability can suffer.
Both patterns affect coordination. One grips too much. The other responds too little.
That’s why strength alone isn’t the full picture. What truly matters is coordination, timing, responsiveness, and the ability to adapt [3].
Signs Your Pelvic Floor Struggles to Relax (“tight” or overactive)
When your pelvic floor has trouble relaxing, your body usually gives you clues. They may feel small at first, but they matter.
Here are patterns I often see:
| What You Might Notice | How It Can Feel |
|---|---|
| Pain with sex or tampon use | Tight, guarded, resistant |
| Trouble fully emptying your bladder | Like something isn’t letting go |
| Constipation or straining | Feels hard to relax and let the stool pass easily |
| Needing to pee often | Urge comes quickly, even if bladder isn’t full |
| Tailbone pain | Achy or sore when sitting |
| Tight lower belly or inner thighs | Subtle gripping you can’t let go |
| Feeling “locked” in the pelvis | Braced, closed, or hard to soften |
| Numbness or diminished sensation during sex | Less enjoyment, and difficulty reaching orgasms |
| Tight jaw or stiff hips | Tension shows up in other areas |
| Feeling like you’re “holding it together” | Always slightly braced |
And here’s something that may not feel logical at first: ongoing tension can still lead to leaking [3]. That’s because when a muscle stays tight all the time, it loses flexibility. Then, when you cough, sneeze, or jump, it may not react quickly enough. So leaking does not always mean weakness. Sometimes it means the muscles haven’t had space to fully soften.
Another common misunderstanding is that if you feel tight, you only need relaxation. In reality, tension and under-activation often exist together. The goal is restoring coordination, besides softening the muscles [6].
Signs Your Pelvic Floor Struggles to Activate (“weak” or underactive)
Now let’s look at the other side of the picture.
When the pelvic floor struggles to activate, the signs often show up during movement. This is when pressure increases and the muscles need to respond quickly.
Here are common patterns I see in this case:
| What You Might Notice | How It Can Feel |
|---|---|
| Leaking when coughing, laughing, running, or jumping | Like support didn’t arrive in time |
| Heaviness or pressure in the pelvis | Dropping or bulging sensation |
| Feeling of collapse during exercise | Unsteady or unsupported from underneath |
| Difficulty “finding” your pelvic floor | Confusing or unclear when asked to engage |
| Clenching glutes or gripping abs to help | Working hard but not feeling stable |
| Inner thighs squeezing during effort | Compensating for deeper weakness |
| Reduced sexual sensation or arousal (difficulty “feeling turned on”) | Less lift, pulse, or responsiveness, or difficulty building sensation |
Here’s the thing: weak does not always mean loose. Your muscles may not feel floppy or stretched out. Instead, they may just have trouble working at the right time. The lift might happen too late. It might be too small. Or the muscles may not work together as a team.
Healthy activation is about responding at the right moment. The muscles engage when needed, and then relax again so everything stays balanced.
Can the Pelvic Floor Be Tight and Weak at the Same Time?
Yes, your pelvic floor can be both tight and weak [1,6]. In fact, it happens more often than most women think [3,7].
A muscle that stays tight all the time cannot create full strength. Real strength needs movement. A muscle has to lengthen, contract, and release to work well. If it stays shortened, it loses power.
Imagine holding your fist clenched all day. Your hand wouldn’t get stronger. It would feel tired and stiff. And when you finally needed it to grip something quickly, it wouldn’t respond well. The same thing can happen in your pelvic floor.
It doesn’t mean something is wrong with you. It usually means your body has been trying very hard to protect you.
This can happen when your body is under stress and stays slightly braced without you noticing. It can also happen when your pelvic floor works hard to prevent leaking or support your organs. For some women, past stress or difficult experiences can also lead the body to hold protective tension in this area.
At first, this kind of holding can be helpful. But over time, it starts to replace natural movement, and coordination fades. The muscles may feel tight, yet they lose elasticity. Their timing gets off. They don’t lift and release smoothly anymore.
So you can feel tense and still leak. You can feel firm, and still lack true support.
But with the right approach, the muscles can relearn rhythm, flexibility, and real strength.
Why Simple Self-Tests Can Help (and Also Mislead)
Self-tests can build awareness, but they cannot tell you for sure whether your pelvic floor is tight, weak, or both [3].
I know many women try simple checks at home. You may have heard of stopping your urine midstream. Or squeezing “as if holding in a tampon.” Some women even look in a mirror to see if the area lifts slightly.
Stopping your urine once can help you notice whether the muscles respond. But doing this regularly is not recommended. It can confuse your bladder’s natural emptying reflex and may increase the risk of bladder problems or infections over time [8].
These tests can help you notice something. You might feel a lift, or you might feel nothing. That information can be useful, but they only show a small part of the picture.
Most self-tests mainly check the outer, more superficial muscles. They don’t assess the deeper layers. They don’t show how the muscles work with your breath. And they cannot measure timing, endurance, or coordination.
There’s another important point: many women are not actually lifting the pelvic floor when they try to do a Kegel. Instead, they may be pushing down without realizing it.
This can increase pressure in the belly and place more strain on the pelvic floor, especially if the muscles are already tight or uncoordinated.
You may also feel effort when you squeeze. But effort is not the same as healthy function. A well-working pelvic floor can lift, respond, and release — not just tighten. Because of this, self-tests can sometimes lead you to try harder instead of moving better.
If you want to understand your pelvic floor more clearly, a specialist can help. Pelvic floor physical therapists and urogynecologists use gentle, structured exams to assess muscle tone, strength, coordination, and relaxation [3,6]. This type of evaluation cannot be done at home.
Working with a specialized pelvic floor physiotherapist is often helpful, as general physiotherapists may not receive enough training in the complexities of the female pelvic floor.
If you live in the United States, you can use this directory to find physical therapists who specialize in women’s pelvic floor health.
If you are based in Germany, you can find physiotherapists specializing in pelvic floor care here.
You may benefit from seeing a specialist if you experience:
Ongoing pelvic pain
Leaking
Heaviness or pressure in the pelvis
Difficulty controlling your bladder or bowels
Symptoms that started after childbirth
A feeling that something isn’t working as it should
Pelvic floor physical therapy is considered a first-line treatment for many pelvic floor problems. It helps restore coordination, relaxation, and healthy muscle function [9].
Building awareness is an important first step. When you begin to feel how your pelvic floor moves and responds, it becomes easier to support it in a gentle and effective way.
My work focuses on helping you reconnect with your body, restore coordination, and create a sense of safety and balance in your nervous system.
You deserve clear answers, and you deserve support along the way.
What Usually Helps First (Before Strengthening)
If the muscles are tight, disconnected, or out of rhythm, adding more squeezing often makes things worse, as it can reinforce gripping patterns instead of solving them.
What helps first is restoring coordination and awareness. Clinical guidelines recommend starting with relaxation, coordination, and neuromuscular retraining before introducing strengthening exercises [9].
This approach aligns with what many pelvic floor professionals are now observing in practice. After participating in the Pussy Yoga Immersion program, pelvic floor physiotherapist Eloïse Deliège explains:
“I’m a physiotherapist for pelvic floor reeducation, and I am questioning what I have been taught during my education. I myself suffered from pelvic floor issues. Now I feel much better in my body. My pelvic floor is better, and the incontinence has decreased by 95%. I began to run again and it’s a delicious feeling. I have changed my way of teaching the pelvic floor to my patients.”
How to do this? I like to think of this in five simple pillars:
1. Curiosity Instead of Control
Many women approach the pelvic floor with a sense of pressure. “Am I doing it right?” “Am I squeezing hard enough?”
But the pelvic floor does not respond well to pressure and control.
Instead, start with curiosity. At first, you may not feel much — and that’s completely normal. Many women need time and guidance to build a clear connection to this part of the body.
Begin by simply noticing your breath and your movement, without trying to fix anything. Over time, as your awareness grows, the sensations become clearer.
You can’t train what you can’t feel.
2. Breath Awareness
Your diaphragm and pelvic floor move together. When you inhale, the pelvic floor expands. When you exhale, it lifts. This natural rhythm is the foundation of healthy function.
Before strengthening, it helps to simply notice this relationship. Breath often restores movement where tension has built up.
If you’d like guidance with this, I include a short 5-minute breathing exercise in my free mini course, where you can follow along and start feeling this connection in your own body.
3. Embodied Perception
Many women describe their pelvis as a “black box.” Rebuilding sensation changes everything. When you can feel the layers, the direction of movement, and the subtle lift and release, the system begins to organize itself better.
4. Gentle, Integrated Movement
The pelvic floor works with your hips, spine, and breath. Simple movements like rocking, walking, squatting, or flowing motion can help restore natural coordination. These movements retrain the system in a way isolated squeezing cannot.
Movement helps your body remember how to work as a whole. This is one reason why I use movement-based approaches like Pelvic Floor Integration™ and Essence of Bellydance™ focused on fluid, coordinated motion rather than force.
5. Nervous System Regulation
Your pelvic floor responds to how safe or stressed your body feels. When you feel tense or guarded, the muscles may stay braced without you realizing it [4].
When your nervous system feels calmer, the muscles can soften, respond, and support you more naturally. This is why regulation comes before strengthening.
This is something I guide you through in my approach, using simple breath and movement to help your body feel safe again and support your pelvic floor naturally.
How Pelvic Floor Integration™ Works
Pelvic Floor Integration™ treats the pelvic floor as part of an integrated whole. It reconnects pelvic floor function with breathing, posture, and nervous system regulation — the processes that naturally coordinate the body in everyday movement.
Instead of focusing on squeezing harder, we restore rhythm, coordination, and responsiveness. This helps your pelvic floor support you without constant effort or tension.
The goal is not just to reduce symptoms. It’s to help you feel more connected, stable, and at home in your body.
“I constantly recommend this approach to my patients because many women feel disconnected from their pelvis, and the focus on embodiment is unique.”
Below is a short guided exercise where I walk you through gentle tailbone (coccyx) activation. This simple movement helps you reconnect with the deeper layers of your pelvic floor (without gripping or forcing):
You’ll find this practice, along with four more mini-lessons, inside the free Body Love mini course in our global community: everything in one place to help you make Body Love a simple daily habit.
Final Thoughts: Understanding Your Pelvic Floor: Why It May Feel Tight, Weak, or Both
By now, you may sense that “tight or weak” tells only part of the story. Your pelvic floor is more than a muscle to strengthen or relax. It is part of your core support system, moving with your breath and responding to posture, stress, and daily life.
So instead of asking, “Is my pelvic floor tight or weak?”, you might ask, “How is my pelvic floor working with the rest of my body?”
You can begin with something simple. Take a slow breath. Notice what happens as you inhale. Notice what happens as you exhale. These small moments of awareness can help restore natural rhythm. If it feels hard to notice anything yet, that’s completely normal. I will guide you through this step by step in a short practice inside the free mini course, so you can start feeling this connection in your own body.
For many women, the real issue is not strength, but connection. Muscles may stay tense as a form of protection. They may respond more slowly when coordination has been lost. This is not a failure. It is often your body adapting to stress, habits, or past experiences.
As breath, movement, and awareness come back into balance, your pelvic floor can begin to feel more responsive and supportive again. From that place, strength develops naturally.
If you’d like a gentle place to start, you can join me inside the free 5-Minute Body Love mini course.
You’ll find a few short, guided practices (each under 5 minutes) that you can easily fit into your day. You’ll also join a supportive community where you can share your experience and feel supported along the way.
About the Author
Coco Berlin is a certified pelvic floor expert, movement therapist, and bestselling author with over 20 years of experience. Her Pelvic Floor Integration™ method has helped millions of women worldwide and is taught in 26 countries.
Frequently Asked Questions About Tight vs. Weak Pelvic Floor
-
It can be hard to tell by yourself. Tight muscles may cause pain, urgency, or a “locked” feeling. Weak or under-coordinated muscles may lead to leaking or heaviness. Many women have signs of both at the same time. A pelvic floor physical therapist can do an exam to clearly check strength, tone, and coordination. With the right guidance, you can also learn to better feel and understand your pelvic floor over time, as we teach inside the Pussy Yoga Immersion.
-
Yes, this is very common [3,6]. When the pelvic floor muscles stay tight for a long time, they lose flexibility and timing. They may feel tight or stiff, but they don’t respond well when you cough or jump. Tight does not always mean strong. Sometimes it means the muscles are stuck in protection mode.
-
If your pelvic floor is already tight, more squeezing can increase tension. The muscles may grip even more.
Another common issue is that many women are not actually lifting the pelvic floor when they try to do a Kegel. Instead, they may be pushing down without realizing it. This can increase pressure in the belly and place more strain on the pelvic floor.
Without learning how to relax and coordinate first, contraction exercises like Kegels can make symptoms worse [6]. The pelvic floor needs to lift and release — not just tighten.
-
No, leaking can happen when muscles are slow or under-coordinated [3]. It can also happen when they are too tight and cannot react quickly enough. Good function depends on timing and balance as well as strength.
-
Yes, stress or trauma can affect the pelvic floor as it is connected to your nervous system [4]. When you feel stressed or unsafe, your body may tighten without you noticing. Over time, this can increase muscle tension and change how the pelvic floor works.
-
You can try it once to get a sense of how your muscles respond, but it’s not something to do regularly.
When you pee, your pelvic floor needs to relax so your bladder can empty properly. If you keep stopping the flow, you can disrupt this natural pattern and make it harder for your body to fully let go.
Over time, this can lead to incomplete emptying or feeling like you need to pee more often.
-
Yes, it can. When the pelvic floor muscles are overactive (high-tone), they may not relax fully during a bowel movement. Instead of gently opening and lengthening, they stay slightly braced. This can change the shape of your stool as it passes through.
Some women notice thinner or flatter stool, difficulty starting, or the feeling that something is “blocking” the way out. You may feel the need to strain, even when the stool itself is soft.
That said, flat or pencil-thin stools can also have other causes. If this change is new, ongoing, or comes with pain, bleeding, or unexplained weight loss, it’s important to speak with a healthcare provider.
A well-coordinated pelvic floor should soften and widen when you relax down. When that release improves, bowel movements often feel easier and more complete.
-
Start gently. Focus on your breath and notice how your pelvic floor moves when you inhale and exhale. Add slow, gentle movements like rocking, squatting, or hip circles. Avoid strong squeezing exercises like Kegels until you get to know your pelvic floor better.
If you’d like more guidance, my free mini-course walks you through these first steps in a simple and supportive way.
References
Nygaard, I., Barber, M. D., Burgio, K. L., Kenton, K., Meikle, S., Schaffer, J., Spino, C., Whitehead, W. E., Wu, J., Brody, D. J., & Pelvic Floor Disorders Network (2008). Prevalence of symptomatic pelvic floor disorders in US women. JAMA, 300(11), 1311–1316. https://doi.org/10.1001/jama.300.11.1311
Patel, U. J., Godecker, A. L., Giles, D. L., & Brown, H. W. (2022). Updated Prevalence of Urinary Incontinence in Women: 2015-2018 National Population-Based Survey Data. Female pelvic medicine & reconstructive surgery, 28(4), 181–187. https://doi.org/10.1097/SPV.0000000000001127
Frawley, H., Shelly, B., Morin, M., Bernard, S., Bø, K., Digesu, G. A., Dickinson, T., Goonewardene, S., McClurg, D., Rahnama'i, M. S., Schizas, A., Slieker-Ten Hove, M., Takahashi, S., & Voelkl Guevara, J. (2021). An International Continence Society (ICS) report on the terminology for pelvic floor muscle assessment. Neurourology and urodynamics, 40(5), 1217–1260. https://doi.org/10.1002/nau.24658
Frazão, L. B., Couto, L. A., Peres, A. C. A. M., Marques, A. P., & Pássaro, A. C. (2025). Assessment of Female Pelvic Floor Muscles: An Integrative Review. International journal of women's health, 17, 2377–2393. https://doi.org/10.2147/IJWH.S532149
Mínguez-Esteban, I., De-la-Cueva-Reguera, M., Romero-Morales, C., Martínez-Pascual, B., Navia, J. A., Bravo-Aguilar, M., & Abuín-Porras, V. (2024). Physical manifestations of stress in women. Correlations between temporomandibular and pelvic floor disorders. PloS one, 19(4), e0296652. https://doi.org/10.1371/journal.pone.0296652
Faubion, S. S., Shuster, L. T., & Bharucha, A. E. (2012). Recognition and management of nonrelaxing pelvic floor dysfunction. Mayo Clinic proceedings, 87(2), 187–193. https://doi.org/10.1016/j.mayocp.2011.09.004
Padoa, A., McLean, L., Morin, M., & Vandyken, C. (2021). "The Overactive Pelvic Floor (OPF) and Sexual Dysfunction" Part 1: Pathophysiology of OPF and Its Impact on the Sexual Response. Sexual medicine reviews, 9(1), 64–75. https://doi.org/10.1016/j.sxmr.2020.02.002
National Institute of Diabetes and Digestive and Kidney Diseases. (2021, November). Kegel exercises. U.S. Department of Health and Human Services, National Institutes of Health. https://www.niddk.nih.gov/health-information/urologic-diseases/kegel-exercises
Torosis, M., Carey, E., Christensen, K., Kaufman, M. R., Kenton, K., Kotarinos, R., Lai, H. H., Lee, U., Lowder, J. L., Meister, M., Spitznagle, T., Wright, K., & Ackerman, A. L. (2024). A Treatment Algorithm for High-Tone Pelvic Floor Dysfunction. Obstetrics and gynecology, 143(4), 595–602. https://doi.org/10.1097/AOG.0000000000005536
Disclaimer
This article is for educational purposes only and is not intended as medical advice or a diagnosis.
If you are experiencing pelvic floor symptoms, it’s important to seek support from a qualified healthcare professional such as a pelvic floor physical therapist or gynecologist.
In our programs, we always recommend working with a professional alongside your practice, so you feel fully supported.
Always listen to your body and reach out for help when needed.